
Practice Perfect 757
The Educational Residency Case Review
The Educational Residency Case Review

Residency education is a multifaceted endeavor in which the academic component is highly important. Consider all of the aspects of education outside of the clinic or operating room. Journal clubs, book reviews, workshops, and conferences all make up a highly important well-rounded residency education program. One aspect of the residency education process that receives relatively less attention is the case conference.
The case conference goes by different names such as case review, radiology review, M&M, rounds, etc. Whatever the name, we’re talking about residents presenting either upcoming cases or cases already completed, and the group discusses these cases. Let’s discuss some aspects of this very important educational episode.
The first thing to understand is that these can be full of minefields. When discussing cases, especially if they are surgical cases with poor results, it is easy to insult someone. Similarly, differences in opinion on procedure choice or patient approaches can become heated, especially if more aggressive individuals are involved. On the other hand, without some preparation and forethought, this type of activity can become a simple show-and-tell activity where the residents don’t learn anything.
To prevent this from happening, here are few suggestions.
- Consider your goals for the activity - The purpose of case conference should include testing resident knowledge and thought processes. This is a great chance to quiz residents of different levels about basic knowledge as well as formatively testing how they think. It should also allow residents to critique outcomes to instill a philosophy of continual process improvement and achievement of technical excellence. There’s something to learn from every case, whether surgical or non.
- Avoid the “show-and-tell” - This is not the venue for residents to compare the last cool surgical case they did – that’s for national conferences where they can go and brag about their great program. Instead, the emphasis is on what can be learned from that case to improve for the next one. This will require the guiding hand of attendings asking good questions such as, “What challenges did you experience during that case?” or “What techniques did you use to make this case go more smoothly?” or my personal favorite, “What could you have done differently?” This is where elucidating important surgical principles yield important teaching points.
- All residents involved should choose cases - This can vary by resident availability, but it’s always a good idea to have all residents present cases (or at least be ready to present). At my program, we ask residents to have at least one case ready to present, while I know that my best residents will always have multiple cases ready to go. Residents should be encouraged to present cases from their non-podiatric rotations and non-surgical cases instead of only discussing their surgical ones. It’s also helpful to be flexible about the length and detail of cases. Sometimes a quick 5-minute discussion about a certain aspect of a case is all that’s needed while in other circumstances, a more detailed discussion with history, physical, imaging, and treatment is needed. Make sure some percentages of cases are ones that have not resolved and then come back to these cases at another case conference some time frame after resolution of the case. This is a great chance to have follow-up and focus on thought process and the results of that thought process later.
- Invite attending physicians - The more people willing to participate the better. We have some regular attendings who participate at the Chino Valley Medical Center program, and their involvement is integral. Earlier in the program, it was only me and an occasional other attending doing these sessions, and I can tell you, it’s a thousand times more beneficial to the residents to have multiple varying opinions from smart and experienced practicing physicians.
- Create a safe environment - This can be a little harder than you might think. Both residents and attendings should be comfortable providing their opinions and admitting ignorance without embarrassment or retribution. There are a lot of personalities involved, and it is easy to say the wrong thing or have someone with hurt feelings. The best we can do is model the behavior we hope to see. One way to avoid this is to keep the names of people involved anonymous. It’s also helpful to maintain both a thick skin and an open attitude toward criticism. No one loves showing their less successful work, but these are the cases with the greatest opportunity to learn and improve.
- Squeeze the marrow out of the good cases - In order for our resident colleagues to learn the most from each case, we need to be comprehensive but also push for follow up and exploration. For example, during the discussion of an ankle fracture ORIF case, residents could be asked to look back at the Ramsey and Hamilton study about tibiotalar contact area (among many many other articles). Almost every topic open for discussion will have some important article in the published literature. This is a great way to link case conference with other academics such as journal club. I also strongly suggest assigning residents to take notes for the group and then share those notes and build on them to create a long-lasting comprehensive resource they can use when studying for board examinations and preparing for future cases.
Here’s a simple example of a surgical case that could be discussed. The details are eliminated for the sake of brevity. Shown below are the preoperative (Figure 1) and postoperative (Figure 2) radiographs of a 40-year-old with painful hallux valgus deformity. Nonsurgical therapy failed and the patient agreed to a surgical approach. Now, before looking at the surgical outcomes examine the preop radiographs. What questions would you typically ask your residents during a case conference? Here are a few options:
- Please read the radiograph - Residents should have an organized approach using proper terminology.
- What abnormal findings do you see? - They should mention findings like an increased IM angle, tibial sesamoid position, and mild pronatory findings, for example.
- Why does this patient have a severe bunion despite the relatively small intermetatarsal angle? - This patient has a significant metatarsus adductus making the true IM angle much greater.
- What procedure would you choose? - The discussion here is usually extensive and variable with lots to talk about including the patient’s needs, whether or not to fix the metatarsus adductus, fusions, osteotomies, etc. It’s always interesting to hear the choices of the less versus more experienced PGY levels.
Figure 1. Preoperative left foot DP and lateral radiographs

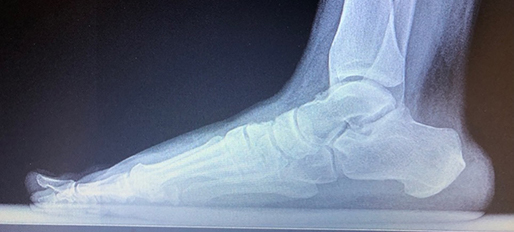
Now look at Figure 2 below, showing the postoperative radiographs. This part of the case conference will yield a variety of other questions. Topics that could be discussed include any of the following:
- Why the modified Lapidus was chosen.
- Choice of fixation method.
- Radiographic signs of union.
- Overall outcomes (congruent joint spaces, proper sesamoid position, shortening of the first met).
- Note the postoperative metatarsus primus elevatus. Topics of conversation, here, can cover if the elevatus is real or an artifact (patient could be lateralizing postop op versus iatrogenic).
- The inquisitive resident might review the literature on the frontal plane bunionectomy procedures (including the contemporary controversy about it), fixation methods (load to failure of double plating systems versus 2-screw versus screw plus plate), and classic articles on the Lapidus bunionectomy (how was it originally fixated? How was the procedure done?).
Figure 2. Nine-week postoperative DP and lateral radiographs


It seems pretty clear that the case conference is a powerful and effective method that provides analysis, improves thought processes, involves dedicated attendings, and grows our residents to be the future physician leaders we want them to be.





























Comments
There are 0 comments for this article